Last updated: June 4, 2026
Having tried PRP and stem cell therapy last year for the severe arthritis and degeneration in my right hip with no improvement, I decided to have a total hip replacement. The surgery was done on March 4 by the amazing Dr. Shane Martin, Director, The Joint Replacement Center of Scottsdale, and Founder, Scottsdale Center for Robotic Surgery (where I had my procedure done). You can read more about the robotic technology here: Benefits of a MAKOplasty Joint Replacement.
Alastair and I checked in at the Center at 6:30am that morning. Surgery prep took several hours. A great team of nurses gave us a thorough briefing of what to expect before, during and after surgery. I drifted away shortly after I was given a spinal nerve block and the anesthesia.


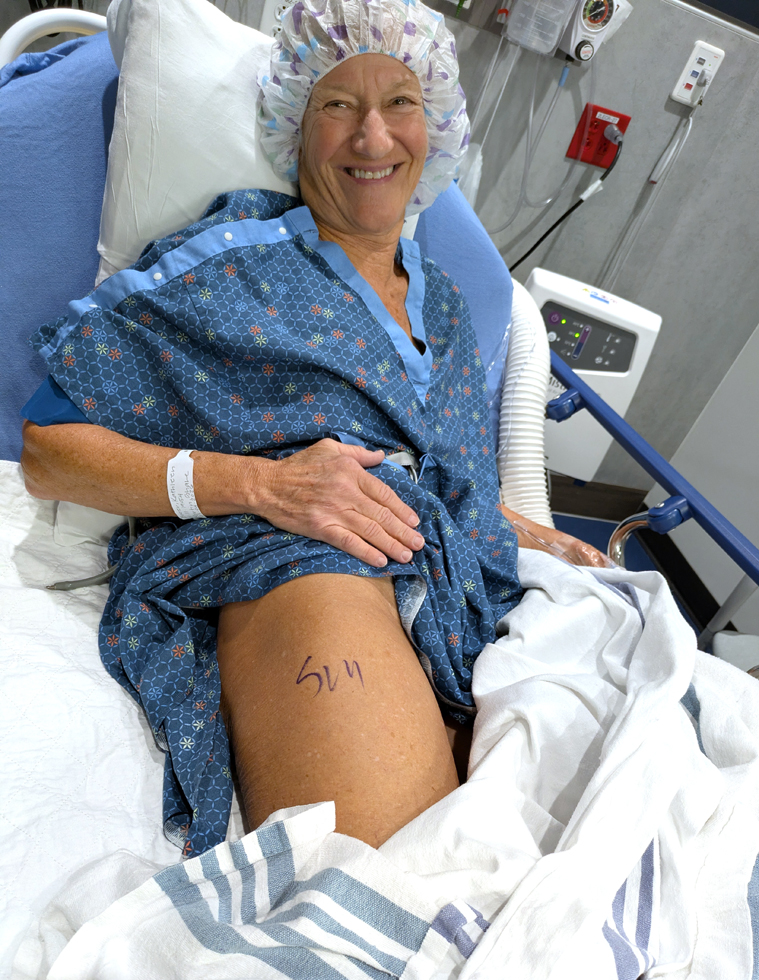
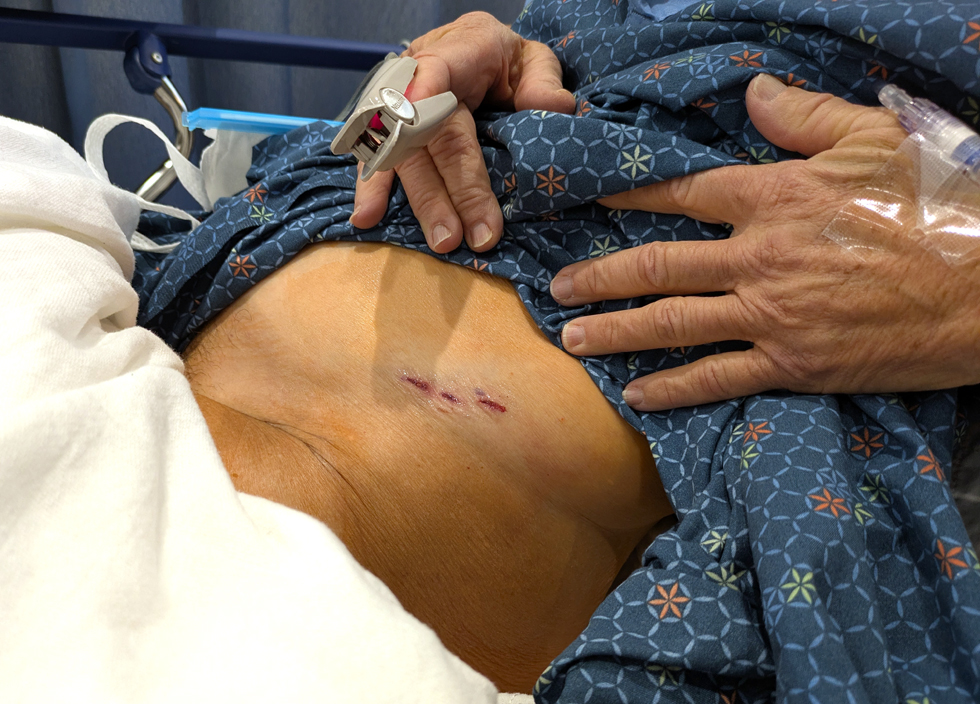
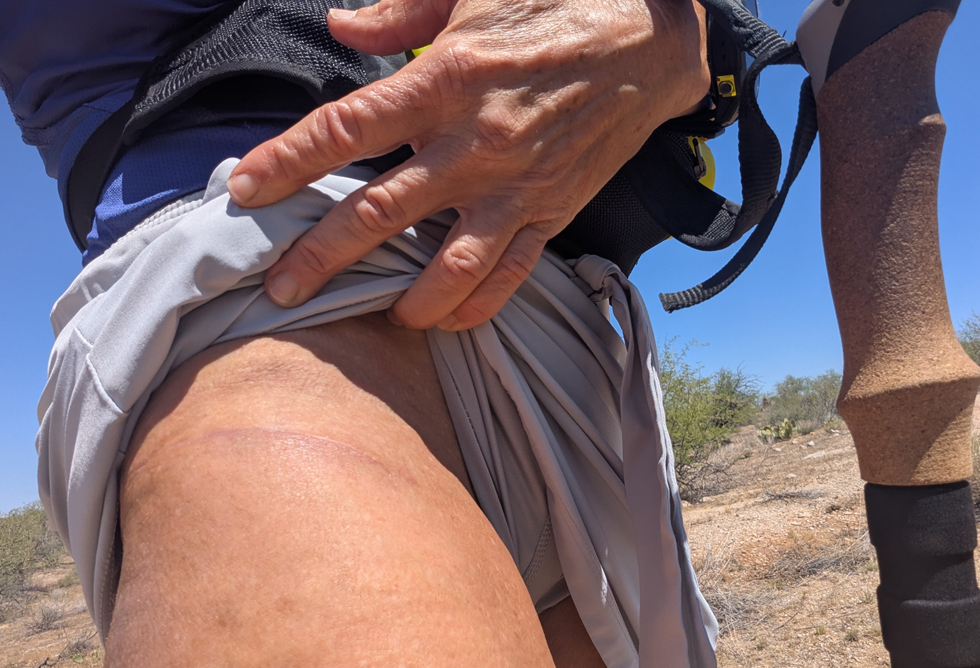
Dr. Martin uses Mako SmartRobotics™ – a surgeon-controlled, robotic-arm assisted procedure for total hip replacement. Using a direct anterior approach, an incision was made over the front of my right hip below the “bikini line”. The incision is shown in 1st image below. This procedure utilizes a muscle spreading technique, which means no muscles get cut, resulting in less bleeding and damage to the soft tissues. The 2nd image below shows where the robotic arm’s optical tracers were attached to my left pelvis, which provided real-time navigation data, enabling implant positioning with a high degree of accuracy. The arthritic ball end of my femur (top of thigh bone) was removed and a metal component (a stem) was inserted into the bone. Then the hip socket was replaced with an acetabular cup lined with durable polyethylene plastic. You can learn more about the Mako procedure on Stryker’s website.


I woke an hour and a half after the surgery, and was almost giddy about how good I felt. Dr. Martin told us everything went very well and judging by the poor condition of my hip there was no doubt that surgery was the right decision.
We left the Center by 12:30pm and went back to our hotel in Scottsdale. I was still drugged up with pain killers so I felt surprisingly good for the rest of the day. I spent the afternoon chilling out… literally! Eating vegan sorbet, wearing a gel ice pack on my hip, and automated compression sleeves on my calves.



We drove home the next day and, not surprisingly, by the afternoon the pain had increased. I was exhausted and apparently the prescription pain med had given my bowels permission to go on vacation (c’mon Miralax, do your thing!).
Friday was much better. Pain level was down, Miralax did its thing, and I was able to walk around more and do the PT exercises prescribed by a nurse at the Center. I was also given multiple products to aid in my recovery: a Manamed Hip Bundle, which includes a cold compression hip wrap, automated calf compression sleeves, and a NMES/TENS device. These devices are used for edema and pain control, as well as DVT and muscular atrophy prevention.
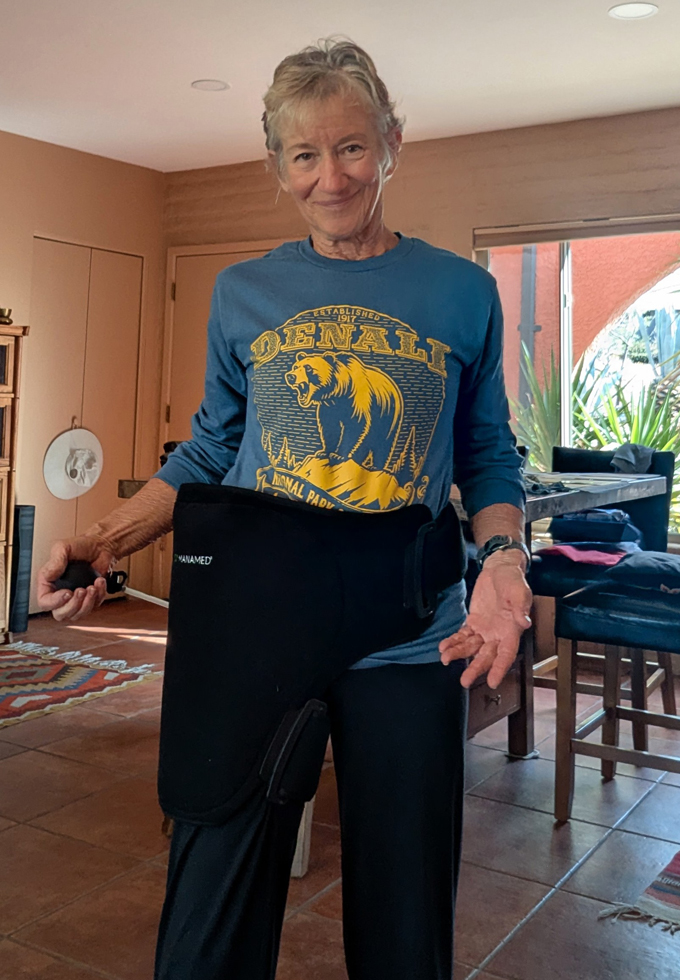



I was also prescribed a number of medications – some required and some to be taken only as necessary. I hate taking unnecessary meds, so as soon as possible I’ve been stopping them: Tranexamic acid, Celebrex, Pregabalin, Hydrocodone, Ondansetron, and Baby Aspirin. By the end of day 3, the only meds I’ve continued to take are Celebrex (anti-inflammatory and pain control) and the baby aspirin (to prevent blood clots).
My recovery continued to go well days 5 and 6. The incision was healing well, no redness or bruising, and less swelling. I started the prescribed PT exercises the day after surgery, and now I’m doing an hour per day of combined PT and upper body strength exercises (gotta stay fit for swimming!). I also started walking with a more even gait, using my hiking sticks as needed – very happy about that! My daily steps counts were the equivalent of 1.5 miles.

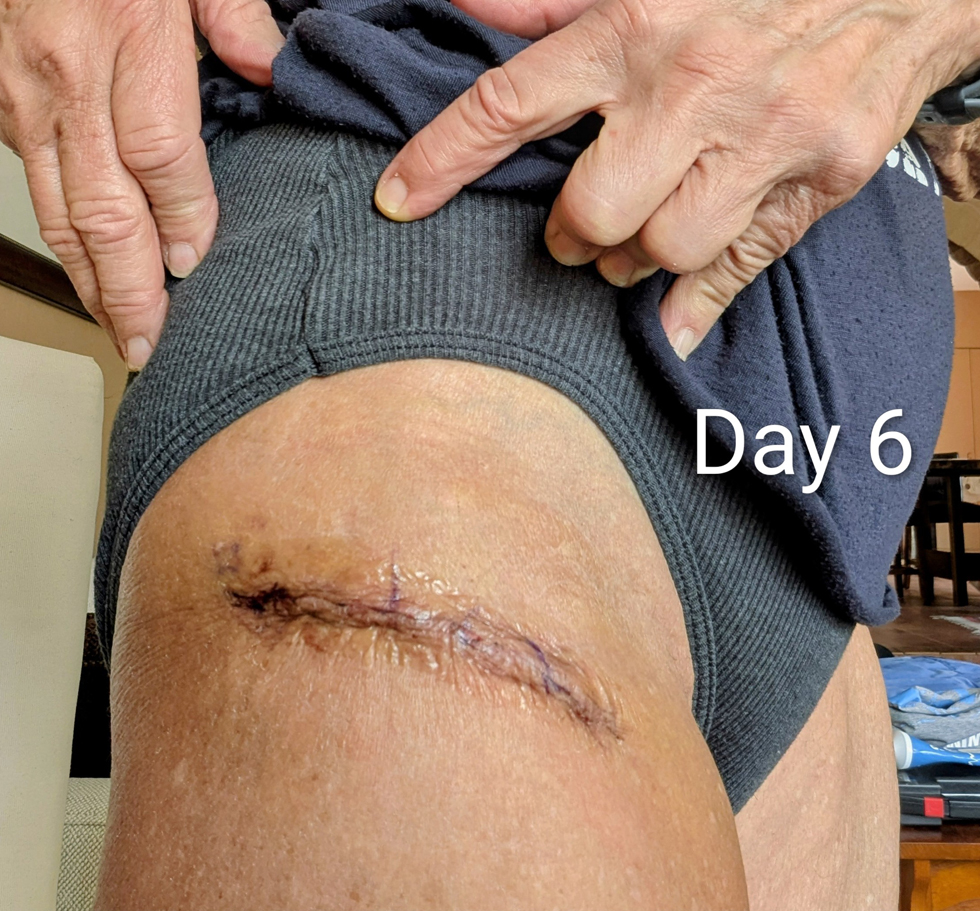
Day 7 was my best yet! I was walking evenly without my hiking sticks, and feeling stronger and emotionally more positive. A home healthcare physical therapist will be coming on Thursday, and my follow up appointment with Dr. Martin is on Friday the 13th – stay tuned!
On the 12th, the home healthcare PT came in the afternoon and did an intake and physical assessment. It didn’t take long for her to let me know that I was doing so much better than most of her patients at this point in their recovery that there was nothing more she could do for me that I wasn’t already doing. She added a couple more exercises, but otherwise said to just keep doing what I’m doing.
The next morning, after doing my PT exercises, a muscle in my inner thigh started to hurt. As Alastair and I were packing for the trip to Scottsdale for my surgery follow up, the pain was getting intense at times. It was frustrating after having done so well over the previous few days, but it was fortunate that it happened before seeing Dr. Martin and not after.
Our appointment at the Joint Replacement Center of Scottsdale started with an assessment and discussion with Dr. Martin’s surgery coordinator. She thought the incision and amount of swelling looked good, but she was conservative with her outlook on when I could resume driving and swimming (the original thought that I shouldn’t swim until 6 weeks after surgery). However, after examining me, Dr. Martin said he was delighted with my progress and said I was good to resume both driving and swimming. YAY!! He said that the pain in my inner thigh was muscular, most likely from the new exercises I was doing: supine straight leg lifts and standing knee lifts. Too soon to do those — he said to take a couple of easy days. Otherwise, everything looked great and we booked our next follow up for mid April, at which point he would review X-rays of my hips to see how the new joint is healing.

March 17, end of week 2, I’m back to swimming at the Oro Valley Aquatic Center!
On Thursday the 19th I went back to my PT Matt Sparrow at Contact Physical Therapy. He was impressed with my progress and gave me some additional exercises. So now I’m doing at least an hour per day of strengthening exercises, plus walking, swimming and using an elliptical trainer at the gym.
A month after surgery I started walking longer distances. On April 1, I walked 4 miles on a relatively flat dirt path. I’ve had very minor pain in my hip, but my right quad and IT band get tight, and that can also cause lower back pain. That tightness can create an anterior pelvic tilt — pulling the pelvis forward and down — which increases the arch in the lumbar spine. This misalignment compresses the lower back muscles, while a tight IT band increases stress on the hips, causing compensating, painful strain in the spine. I told my PT about it this week and he gave me additional stretches to help relieve the tightness. I also do myofascial release on my quad using a roller stick, as well as electrical stimulation and a massage gun. It helped enough that I felt up to trying a longer hike (ignoring my PT’s advice to not overdo – haha, he knows me better than that).
On Saturday, April 4, Alastair had an orienteering event at the AZT trailhead that is the beginning of my section of the Arizona Trail (I’ve been the steward for many years). His event took most of the day, so I went off to hike, stopping often to stretch, take photos, and do a bit of trail maintenance (cutting back catclaw – a desert shrub known for its sharp, hook-like thorns). I did 5 miles with roughly 400 feet of elevation gain. I actually found doing a bit of climbing was more comfortable than my previous walks on flat, dirt path – which makes sense since it requires using a mix of different muscles. The next day I had some aches, but I did my PT exercises, iced, and stretched. By midday I was feeling pretty good!


April 10 was a telehealth call with Dr. Martin to review my recent x-rays. He said everything looks great and is healing very well, so he said I can start ramping up my activity level. Great news!
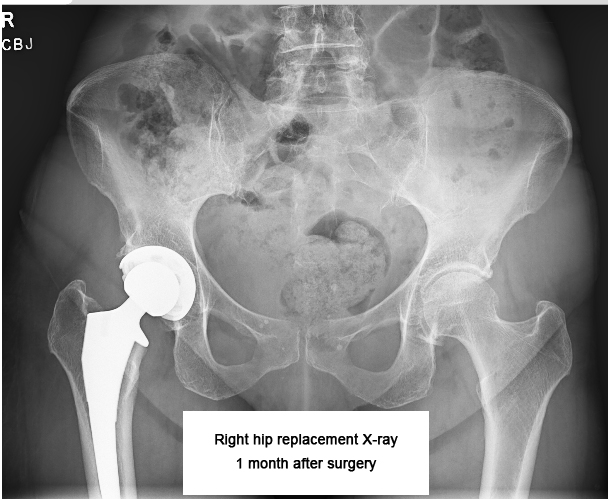
I’m now hiking longer distances, with more elevation gain and on more technical trails. I was on a trail near our home on April 12 – I took it easy but felt pretty good! As long as I remember to take days to recover, I should continue to improve.

At 9 weeks after surgery, I’ve been able to resume all of my regular activities, although still trying to “take it easy”. Road cycling is less painful as long as I don’t have to make any sudden stops or climb steep grades. I even tried a little bit of trail running… to be clear it was more of a fast shuffle…but no pain during or after. Especially satisfying was participating in an Arizona Trail work event on April 29, helping to build a new section on Passage 5. Great to see friends, some of which have also had joint replacements and are doing very well!



Final update June 4:
At 3 months after surgery, I’m thrilled to report that recovery has gone better and faster than expected! I’m now ready to take on some new adventures. So what am I thinking? An aquabike event in Flagstaff in August, and then traveling with Alastair to Europe in the fall (Scotland, Switzerland & Spain), primarily to visit family and friends. I’m even looking at events for next year – possibly doing the Amtrak Century Ride in California with my brother in May, and then traveling to Georgia and Florida in June. More about these later in separate posts!
