Last updated: October 9, 2025
Regenerative therapy offers several potential benefits, primarily focusing on tissue regeneration, pain reduction, and avoiding or delaying surgery. By harnessing the body’s natural healing abilities, it can help repair damaged tissues, reduce inflammation, and improve overall function and mobility. I’ll explain what led me to consider regenerative therapy.
In November 2024, two months after my Half Ironman in Santa Cruz, I started experiencing significant right hip and lower back pain that stopped me from running. Over the years, I’ve had occasional pain in these areas due to hip arthritis and spinal disc degeneration, but this was more disabling than before. I also have knee arthritis and mild scoliosis. I’ve seen traditional orthopedists without any positive results – like most doctors, they either want to prescribe medications or advise surgery. Not options I favor. Physical therapy and strength training have always produced the best results; but unfortunately, that doesn’t build new bone or repair degeneration. After several months of PT at the beginning of the year, my condition had not improved.
In 2023, Alastair and I were training for our first ultra trail run and at that time knee pain was my main problem, but I also had occasional hip and back pain (and you ask, “why do you do these things?” haha). I consulted with a new doctor, John Tait, of Origen Orthopedics. Dr. Tait injected my knees with hyaluronic acid, the natural lubricant found in your joints. A month later, I was running again without knee pain. Because of the success of that, I started discussions with Dr. Tait about PRP and stem cell treatments for my hip and back (neither of which are coverage by insurance). Given the high cost, I decided to start conservatively, and do a PRP treatment only in my right hip.
January 2025
Platelet-rich plasma (PRP) therapy involves using a concentrated solution of a patient’s own platelets to promote healing and tissue regeneration. The blood is processed to concentrate platelets, which are then injected into an injured area. I had the procedure done at Origen on January 28. The procedure itself was painful, but bearable. I had both PRP and an adipose fat injection (both blood and fat were harvested from my body). PRP, derived from the patient’s own blood, contains growth factors that promote healing. Adipose tissue, harvested from the patient’s body, can be used to provide cushioning in the hip area.
I was asked if I wanted a prescription pain medication, but having not been through this before I underestimated how severe the pain would become. That night and the next morning the pain felt like 12 out of 10! I had the doctor call in the prescription and started taking it later that morning. Even with the meds, I had difficulty walking the first 2 days.
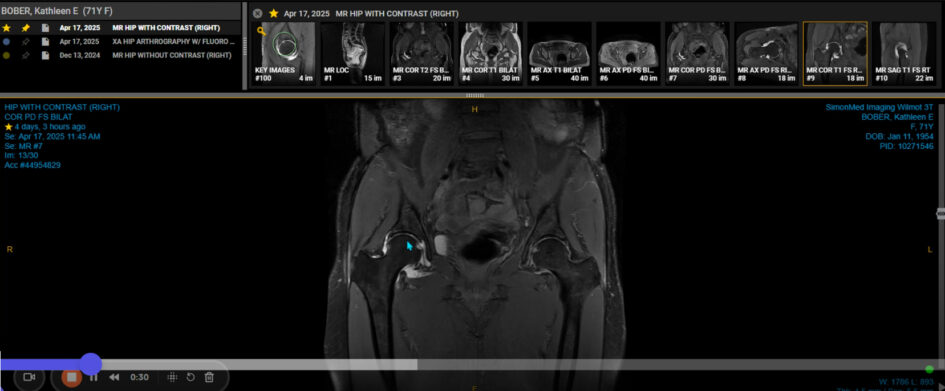
The following week, I started swimming with a pull buoy, doing light upper body weight training and some gentle yoga. The recovery guidelines generally advise taking it easy the first 2 weeks, then starting PT at week 3, which I did. By mid March, I started cycling short distances, which caused no additional pain. By mid April, I resumed taking some classes at the YMCA, both strength and yoga, but certain movements were increasing my hip pain. I contacted Dr. Tait and he ordered a hip MRI with contrast.
A hip MRI with contrast, also known as MRI arthrography, is a specialized imaging technique used to visualize the structures within the hip joint in greater detail. It involves injecting a contrast agent, usually gadolinium, directly into the hip joint before taking MRI scans. This helps to highlight the labrum, cartilage, ligaments, and other soft tissues, making it easier to identify injuries or abnormalities. My MRI results showed no evidence of osteonecrosis, moderate to severe OA, and labral degeneration without flap tear (the blue arrow in the 2nd image points to the area of labral degeneration).
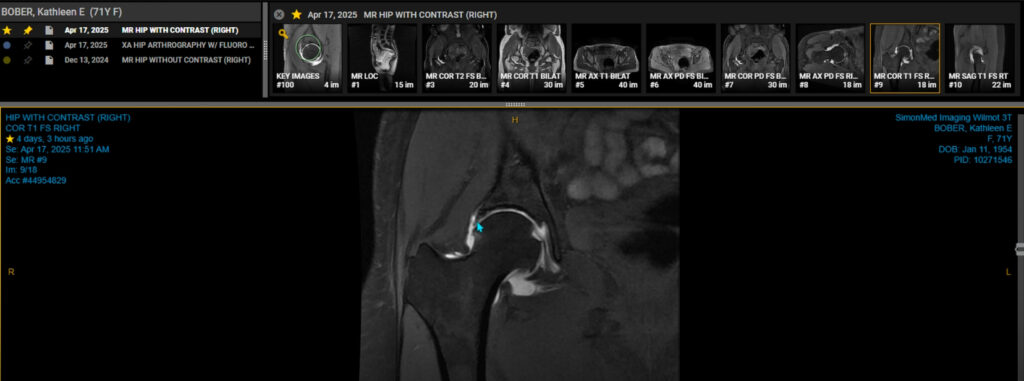
Based on this, Dr. Tait suggested some regenerative therapy options: 1) do a PRP “boost”; 2) inject 2mL exosomes; or, 3) inject PRP + 2mL exosomes. To be clear, exosomes are simply stem cells, which are found in many tissues, including bone marrow, adipose tissue, and umbilical cord. Dr. Tait said the majority of his patients opted for cells from birth tissue, since the idea of “drilling into their bone” for marrow was frightening.
Since it had been 12 weeks after the PRP treatment and I had no improvement in pain, I decided to do more research and consult with other doctors. A doctor in Phoenix said (and this was supported by multiple other sources) not to do birth tissue… “It’s unreliable and nobody checks to see if cells are still alive.” Alastair assisted with my research by utilizing AI and Gemini Deep Research to produce several documents on stem cell therapy and some of the doctors I was considering.
As a result, I decided to have the procedures done by Dr. Stephen Derrington, of Derrington Ortho in Carlsbad, CA. Dr. Derrington has been a member of the Regenexx network since 2016 (which is how I found him), and among his key achievements are top Regenexx performer in CA and 3rd in US (2023).
July 2025
Alastair and I went to Carlsbad for a week. We arrived the day before my first procedure, so we took advantage of what would probably be my last mobile day to visit the ocean and a brewery (just NAs for me for the next several months – doing everything I can make the procedure a success by reducing inflammation).



My first procedure on Monday, July 7, was for the stem cell injection in my right hip. Blood was drawn and then, using local anesthesia, the doctor collected bone marrow. Bone marrow is harvested with a trocar, which is a surgical instrument used to access and collect bone marrow from the iliac crest or other bones. It’s essentially a specialized needle designed to penetrate bone and create a pathway for aspirating or collecting bone marrow. Dr. Derrington took out 90cc (9 draws of 10cc). The goal is to have than 600 million stem cells, and I had 1.6 billion, meaning I had 96% viability (which refers to the percentage of living, healthy cells in a stem cell population).

My pain expectation during the procedure was based on my previous PRP treatment, and it was about the same – painful but bearable. And given what I knew about how the pain ramps up over the following 24 hours, I took a Percocet soon after the stem cell procedure, which helped enormously. I never had quite the same difficulty walking as I did after the previous PRP procedure. What I totally underestimated was the affect the pain med would have on my gut – I was severely constipated for several days!
On Thursday, July 10, I had the PRP treatment done on my hip and lumbar spine. Again, blood was drawn first and then processed to isolate and concentrate the platelets, which were then injected back into me. This process aims to harness the healing properties of platelets, which contain growth factors that can promote tissue repair and regeneration.
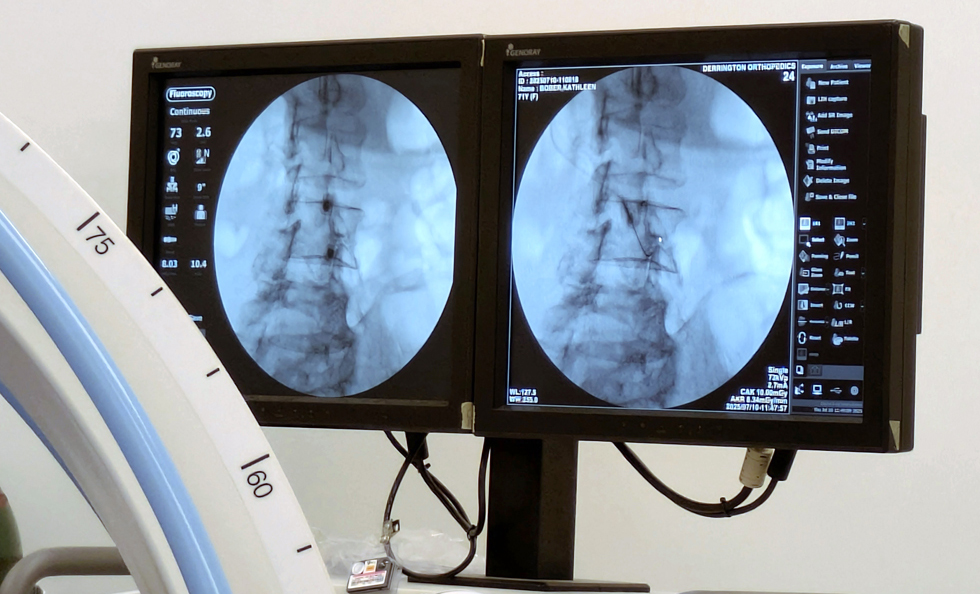
Pain after this procedure was minimal, but we went back to our room and took it easy. Fortunately, I got almost 9 hours of sleep that night. Unfortunately, I was still dealing with severe constipation, which turned to diarrhea by the next day. Ugh!! I’m so grateful to Alastair for all his love and support during this ordeal… running out to get me anything I needed even though he was still working remotely from our room most days.
By Friday evening, I was feeling much better and dying to get out of the room, so we went to Arcana Brewing. Fantastic place! Cool vibe, great owner, and it seemed almost all of the patrons were regulars. We liked it so much we went back Saturday evening. I appreciated that they had a nice selection of both IPAs and non-alcoholic beers, so Alastair and I were both happy.



We returned to Tucson on Sunday, July 13. The drive was uneventful, which is good, and I was even able to share driving with Alastair. I didn’t great sleep that night or the next, I’m not sure why but it wasn’t because of pain. I hadn’t used any pain medications since the morning of 7/9, but I’m now regularly using things that Dr. Derrington included in cost of treatment: Incrediwear Back Brace, Incrediwear Hip Brace, Thermotex Platinum Infrared Heating Pad, and Küribl Klinical Muscle Cream with 3000mg CBD (not shown). All of these have helped enormously!


As of this writing, July 21, I’m starting week 2. It’s still too early to tell if the procedures have been successful – it can take 3 to 6 months for someone to be back to their “normal” activities at 100%. That’s the length of time the regenerative component happens, whereby the cells make collagen and the proteins that constitute cartilage – that takes time.
We’re all different, so what’s normal for me may not be the same for someone else. You just have to look at some of my other posts to see that I love being active. I’m happy to say that I’ve been able to resume swimming 4x per week, my weekly step count has been the equivalent of 20+ miles, I’m doing gentle yoga, using the elliptical machine at my gym, and doing some resistance training. I tried a short hike in Catalina State Park yesterday on a level trail, but my right hip and IT are still painful. I’ll be starting physical therapy tomorrow, so I’ll update this post at week 3 and hopefully can report good progress.
Update: July 29
It’s been 3 weeks since the procedure, and while there have been improvements I’ve also had a few not so great days, which was to be expected. Those days are usually attributed to doing too much, which unfortunately I don’t realize until after I’ve done “too much.” Doctors and PTs always say “let pain be your guide” – um, great… but it doesn’t hurt at the time, just after. On the plus side, I’m usually back to my baseline pain of 1-2 out of 10 within a couple of days.
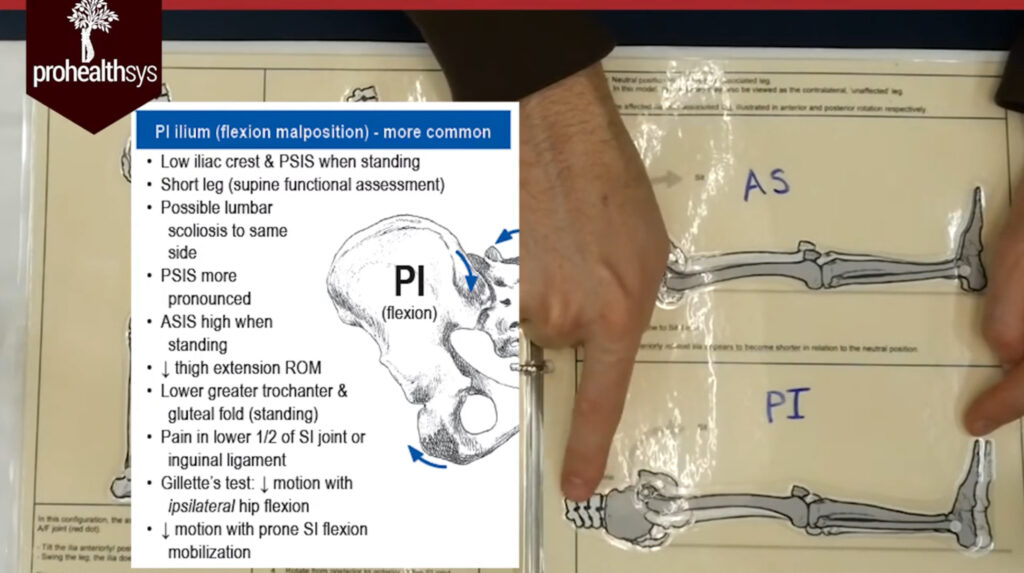
Last week I had my first PT session with Matt Sparrow, whom I worked with in 2019-2021. One of the assessments he did was the “supine to long sit test” (none of my recent PTs have done this). He discovered I have a functional leg length discrepancy. During this test, leg length can appear to change when transitioning from a supine (lying on your back) to a sit-up position. This is where the apparent difference in leg length isn’t due to differences in bone structure but rather to the position of the pelvis or muscle imbalances. The result of my test revealed that I have a posterior pelvic rotation – my right leg appears shorter in the supine position and lengthens as I sit up. This lengthening occurs because the hip flexors activate during the sit-up, anteriorly rotating the hip and moving it towards its normal position. The altered position of the acetabulum (hip socket) due to the posterior rotation makes the leg appear shorter in the supine position. This is a great YouTube video that demonstrates the hip movements during the test.

Matt gave me a series of exercises that are intended to help correct this. I diligently did them twice a day for the first week. In today’s PT session we repeated the “supine to long sit test” and the result was an astounding correction in my leg length! In both the supine and the sitting up positions the length of my right leg was even with my left. Matt was quick to say that just one week of these exercises would not produce a permanent fix. Most likely, I’ll need to incorporate these targeted exercises in my regular routines for the rest of my life. But, hey, they work, so that motivates me to continue, which hopefully will alleviate some of my pain. My instructions for the next week are to continue doing the same exercises, but increase the number of sets. I’ll continue to report my progress!
Update: July 30
Today was a particularly great day with a trip to Patagonia Lake State Park for a swim, and then to my section of the Arizona Trail on Passage 4 on the east side of Mt. Wrightson for a bit of trail work. I woke almost pain free, and felt even better by the time I got home in the afternoon. YAY!! Let’s hope these good days continue!

Update August 8
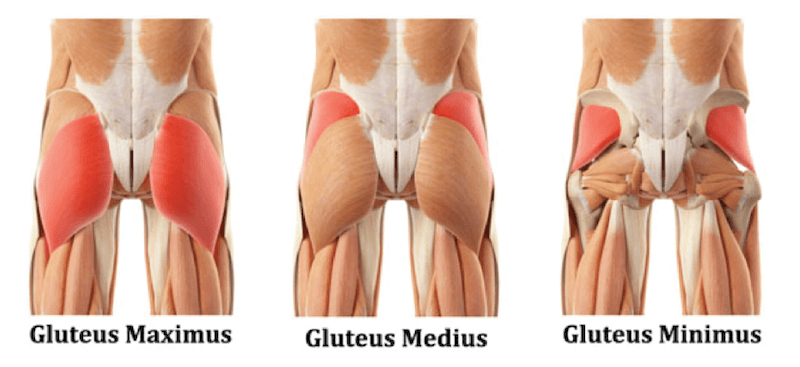
Progress continues, but slower than I would like (of course). A week ago, I got a message on Origen’s patient portal from Dr Tait, with a revision to his diagnosis of my hip MRI done in April (hmm…why now, I wondered). He now lists gluteal tendinopathy as one of my conditions, where he didn’t mention it at my follow up in April. Regardless, I told my PT Matt Sparrow this week about it, and he said that tendinopathy of the gluteus medius would make sense given my pain symptoms. This image shows the glute muscles:
Per an article on the Royal Orthopaedic Hospital website, “Gluteal Tendinopathy is a term that describes any problem with the gluteal tendons. In this condition the tendons are not normally inflamed… Most experts accept that the problem is degenerative… however for most people it is a rectifiable issue. Put simply, the body is constantly being strained (causing wear) with activity and repaired during rest. If the rate of wear becomes faster than the rate of repair, then healthy tendons can start to become weaker, until the point they become painful. Many issues affect this wear and repair process such as exercise loads, fitness levels, body fat, hormonal changes, stress, postures and limb alignment, and previous injuries. Therefore gradual re-introduction of activity alone does not always work and more specific rehabilitation is needed. This rehabilitation will look to identify the factors contributing to the problem and build a specific exercise programme to strengthen the gluteal muscles and tendon, to improve their tolerance to activity. The rehabilitation process often takes months as tendons do not have a rich blood supply, meaning adaptation to exercise can be slow. In the majority of cases however, if you are compliant with the exercise programme and patient, this approach is successful and leads to long-term successful outcomes.”
So, has my PT built a specific strength exercise program by identifying the factors contributing to my problem(s)? Yes. Will I be compliant with the program? Absolutely, yes!
Between the stem cell / PRP procedure and gluteal tendinopathy, my recovery process will undoubtably take months. Will I keep a good attitude even on those painful days? I’ll try. 🙂 More later…
Update: August 12
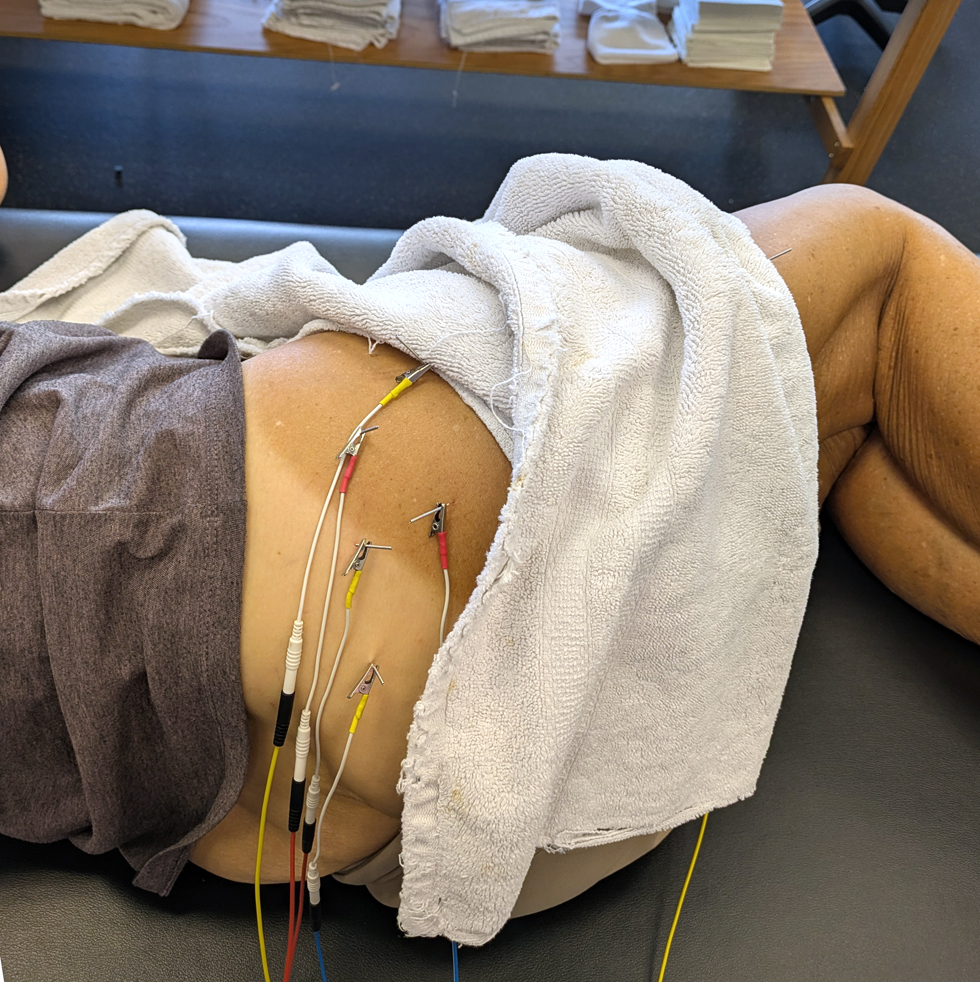
Since my last PT session a week ago, I’ve had overall less pain with more good days than not so good. During today’s session, Matt tested my hip strength and congratulated me on making significant gains! To help alleviate pain, he suggested dry needling with electrical stimulation. Dry needling involves inserting fine needles into specific myofascial trigger points – the goal being to reduce localized tension, improve blood flow, and alleviate pain. Electrical stimulation enhances the effects of dry needling by sending low-frequency electrical currents through the needles. This creates muscle contractions, promoting relaxation and increasing neuromuscular activation. In my case he inserted 6 needles in key hip muscles: iliopsoas, and glute min, med and max. The treatment lasted 15 minutes.
The result was impressive! Pain-free for the rest of that day, and minimal for the next 2 days. I’ll certainly do another DN with e-stim treatment next week!
Update: August 15
Dr. Derrington had suggested that I might find extracorporeal shock wave therapy (ESWT) helpful with the stem cell healing process. “ESWT is a non-invasive intervention that creates sound or pressure waves that propagate through tissues to stimulate interstitial and extracellular responses (Source).” It works by promoting the formation of new blood vessels, activating cells responsible for tissue repair, and breaking down scar tissue.
I found two options in Tucson and one in Tempe (which was recommended by Dr. Derrington). I was able to get an appointment today with Dr. Courtney Davis at Resiliency Wellness, who uses SoftWave Therapy. Their introductory offer was $69, so I figured I’d go for it. I had a brief consultation and evaluation with the doctor, and then a 10 minute shockwave treatment, which focused on the areas of pain in my right hip, groin and IT band. The pain was intense when it hit my trigger points, but the intensity was easily adjusted to make it more tolerable. I’ll withhold judgement on the effectiveness for a few days, but I will say that when walking back to my car after the treatment I felt the pain was more intense in my right IT. I don’t plan to have another treatment while I’m doing dry needling with electrical stimulation with Matt Sparrow – I want to be able to judge how well that works before I start another type of treatment. So, again…more later.
Update: August 19
Significantly better this week – multiple days with pain 0-1 out of 10! Had another treatment of dry needling with electrical stimulation at PT today. Can you believe some of the needles go into my body as deep as 4″? It’s impossible for me to tell. But, wow! What a difference – so much better after.
Update: August 27
Well, the “so much better” after last week’s needling with stimulation didn’t last long. In fact, I had some of the worst pain since my stem cell procedure for the following two days (but gone by the 3rd day), primarily in my right tensor fasciae latae (TFL). “The TFL works in conjunction with the gluteus maximus, gluteus medius, and gluteus minimus in a wide variety of hip movements, including flexion, abduction, and internal rotation.” (Source).
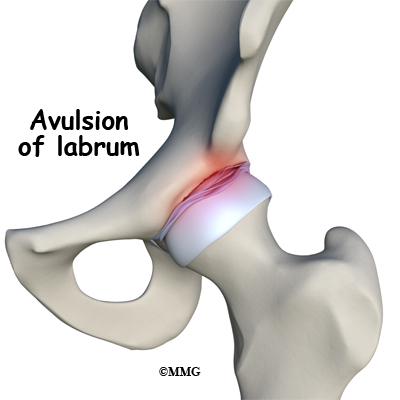
Due to my multiple conditions (hip arthritis, labrum degeneration, gluteal tendinopathy), my TFL is forced to work harder to provide stability, which leads to significant tightening. So why the increased pain after needling? My PT Matt thinks the treatment was so effective at temporarily halting the tightness and guarding in my TFL, that it actually made me feel more pain coming from my hip joint. And due to my symptoms and where I often feel pain, we believe it’s primarily caused by the labral tears (avulsion). As Dr. Derrington explained it, “Think of the labrum like a rubber gasket, which can get dry and cracked over time. These types of tears can’t be surgically repaired/tied together, only debrided and cut away.”
Debridement simply means that the torn or weakened portions of the labrum are removed. This prevents the torn fragments from getting caught in the hip joint and causing pain and further damage to the hip joint.
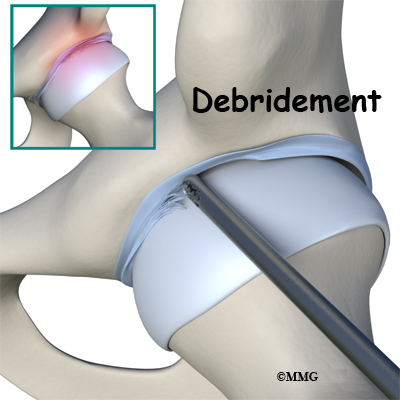
So ultimately, I may need surgery – but that can wait. In the meantime, I’ll continue with strengthening the surrounding muscles and try not to make it worse by doing high-impact exercises, such as running.
Update: September 9
Alastair uses Gemini Deep Research both professionally and personally, and suggested that we use it to further explore the multi factorial causes of my pain. Then ask it to provide a research paper with recommendations.
To do that, you assign a role to your personal AI research assistant, provide it with relevant information about your conditions, diagnoses, treatments, lifestyle, etc. Then create a prompt…meaning tell it what you want to know. You can continue finessing the prompts until you feel you have all the information you need.
The reports it produced were amazing and very helpful, but too lengthy to post here. But what I will share is the Deep Dive podcast we asked it to create. Have a listen! It’s hard to believe it’s AI generated!
Untangling the Hip-Spine Syndrome – Why Your Persistent Pain Might Be a Spinal Mystery
Update: October 9
Alastair and I returned this week from 5 weeks abroad (details in another post). The travel went well, and over the 5 weeks, we walked or hiked more than I have all year, totaling @ 160 miles. I kept up with my daily PT and resistance training exercises, missing only one day the entire time. I was only able to swim twice, and no cycling. Overall, pain was not bad. We did several 5+ mile hikes, and often I used a hiking stick. My pain was mostly in my right IT and right knee, but usually resolved by the next day. The pain was usually the worst when we walked on pavement, or prolonged standing (like in museums).
I’m undecided about how much I’ve benefited from my regenerative therapy treatments. Unfortunately, I think there are multiple conditions causing my pain that these treatments were unable to address. Was it worth it? I’m not sure yet. I’ll be meeting with my PT on 10/15, and then have a follow up call with Dr. Derrington on 10/17. I’ll update the following week.
Update: October 18
I had my last PT appointment with Matt Sparrow this week, and we agreed that there’s nothing more he can suggest to do that he hasn’t already. We did strength tests and he said I’ve greatly improved, and that I’m at the highest level I can be given my conditions. He also said that I’m light years ahead of some of his other clients with even less degeneration than I have. Great to hear, but doesn’t do much to alleviate my pain. He told me about a great orthopedic surgeon who he knows personally, Dr. Timothy Dixon – his mother and many of his clients have have great success with his joint replacements. The next day I booked a consultation for late January, and will consider a hip replacement if there’s nothing else that can be done.
On 10/17, I had a follow up phone consultation with Dr. Derrington. Clearly he was disappointed that the stem cell and PRP treatments have not helped. He agreed that having a consultation with an orthopedic surgeon would be a good next step. Given my the degeneration of my spine and the mild scoliosis, he also agreed that we need to do more diagnostics to figure out what contributes most to my pain – my spine or my hip. To do that, he said I should ask for a diagnostic hip injection (just with anesthetic/numbing medicine, and ideally no steroid/cortisone – the purpose is to determine if my hip is the primary source of my pain.
So at this point, I will sadly say that degenerative therapy has not worked for me. But I still feel it was worth trying.